From Livestock to Intimate Contact: A Rare Animal Skin Condition Emerges in Gay Men
A rare skin infection normally seen in sheep, horses and cattle is now being reported in sexually active men, prompting concern among public health officials. The United States Centers for Disease Control and Prevention (CDC) has documented nine cases of the condition — known as dermatophilosis or “rain rot” — in men diagnosed in Barcelona, with further clusters identified in Lyon, Paris and Germany. All of the men reported having sex with other men, and none had any known contact with infected animals, a significant departure from the disease’s usual transmission route.
From Zoonotic Disease to Sexual Transmission
Dermatophilosis has long been classified as a zoonotic infection, meaning it typically passes from animals to humans. The bacterium responsible, Dermatophilus congolensis, is an unusual pathogen that exhibits characteristics of both bacteria and fungi. It thrives in wet conditions and is commonly associated with rainy seasons, which is how it earned the name “rain rot.” In livestock, it produces crusty, scabby patches and matted hair, often on the back, legs or face. Human infections have historically occurred through direct contact with infected animals — farmers, veterinarians and horse handlers are considered most at risk. The bacteria can also survive on contaminated surfaces such as grooming tools and brushes.
Dr Lawrence Cunningham, a clinician speaking on behalf of UK Care Guide, notes that “from what I’ve seen, it’s almost always farm workers or vets who pick it up, and usually after repeated or prolonged contact rather than a single brief touch.” He adds that “most clinicians could go their entire career without seeing a confirmed case.”
However, the recent European outbreaks represent a striking epidemiological shift. The CDC has pointed to the infections being “sexually acquired,” and research published in Emerging Infectious Diseases detailing the Barcelona and Lyon clusters found that genetic sequencing showed a close relationship between strains from the two cities. All affected men were men who have sex with men (MSM), and several reported partners with similar symptoms. Lesions were commonly located on areas exposed during sexual contact, including the genitals, thighs, groin and face. Crucially, none of the men reported animal exposure.
Eight of the nine Barcelona patients said they had visited a sauna or similar venue for sexual encounters shortly before developing symptoms. The humid conditions in these spaces are believed to favour the growth and transmission of the bacteria. The pattern of spread through sexual networks has drawn comparisons to the early stages of the 2022 mpox outbreak. “Given these recent reports about transmission in certain communities, I’d point to intimate contact,” Dr Cunningham explains. “Prolonged skin-to-skin exposure where the bacteria has enough time to transfer and take hold.” He notes that while human-to-human transmission is even rarer than zoonotic infection, the new evidence suggests it is possible through direct skin contact, especially in environments that help the pathogen survive.
The bacterium can also enter through cuts or abrasions on wet skin, making intimate contact in saunas a plausible vector. All men in the study had high exposure to other sexually transmitted infections, further supporting the theory of sexual acquisition. While the condition could technically fall under the STI umbrella, Dr Cunningham stresses that it does not behave like chlamydia or gonorrhoea.
What Is Rain Rot and What Are the Symptoms?
Medically known as dermatophilosis, the infection is caused by Dermatophilus congolensis, a bacterium that can survive in both wet and dry conditions. In humans, it typically presents as an itchy, folliculitis-like rash. The men diagnosed in Europe experienced a range of skin lesions: papules (solid raised bumps), vesicles (small fluid-filled blisters), pustules (pus-filled pimples), crusts, scabs, nodules (abnormal lumps) and scaly lesions. These are generally not serious but can cause significant discomfort.
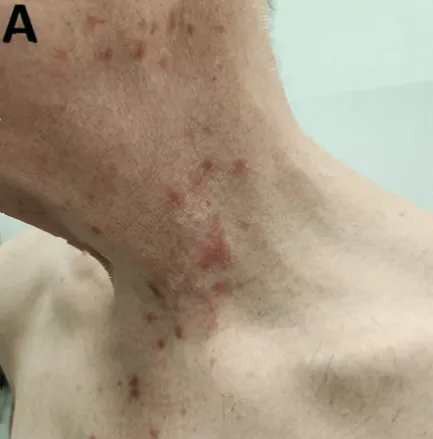
“What rain rot does is create crusty, scabby patches on the skin that can get quite uncomfortable if left alone,” says Dr Cunningham. The main concern is secondary bacterial infection if the skin becomes damaged, particularly from scratching. “Left untreated, there’s a small risk of the infection reaching deeper tissues,” he adds, “but with proper medical attention, serious complications are rare.”
The incubation period for dermatophilosis is typically one to four weeks after exposure, with symptoms often appearing within the first two weeks. In the European outbreak, symptoms typically emerged around the sixth day.
Treatment, Risk and Public Health Outlook
Diagnosis is straightforward. “Doctors can diagnose it through skin samples or bacterial cultures,” Dr Cunningham explains. “It’s straightforward testing, and most labs can identify the bacteria without difficulty.” Microscopic examination of skin crusts and culturing the organism are definitive methods.
Treatment relies on antibiotics. For localised patches, topical antibiotic creams are usually sufficient; more extensive cases may require oral antibiotics. Most reported human cases have been mild and resolve easily, either spontaneously or with standard antibiotic therapy. “Antibiotics are the best way to treat this initially, and they work well when you catch it early,” says Dr Cunningham.
Nevertheless, there is concern about how the infection might present in immunocompromised individuals, such as those with uncontrolled HIV. The World Health Organization (WHO) is aware of the European cases but currently assesses the risk of widespread epidemic levels as low. However, the situation highlights the possibility that human dermatophilosis may be underdiagnosed, particularly in patients with animal contact or in communities where it is not typically expected. Clinicians, especially those in sexual health settings, are being urged to consider the infection when investigating unexplained skin lesions.
Good hygiene practices — including thorough handwashing after animal contact and maintaining cleanliness in shared spaces such as saunas — are recommended as preventive measures. Dr Cunningham emphasises that “dermatophilosis is very treatable and still quite rare, and public awareness just means you’re more likely to seek help early, which is exactly what makes the difference.”