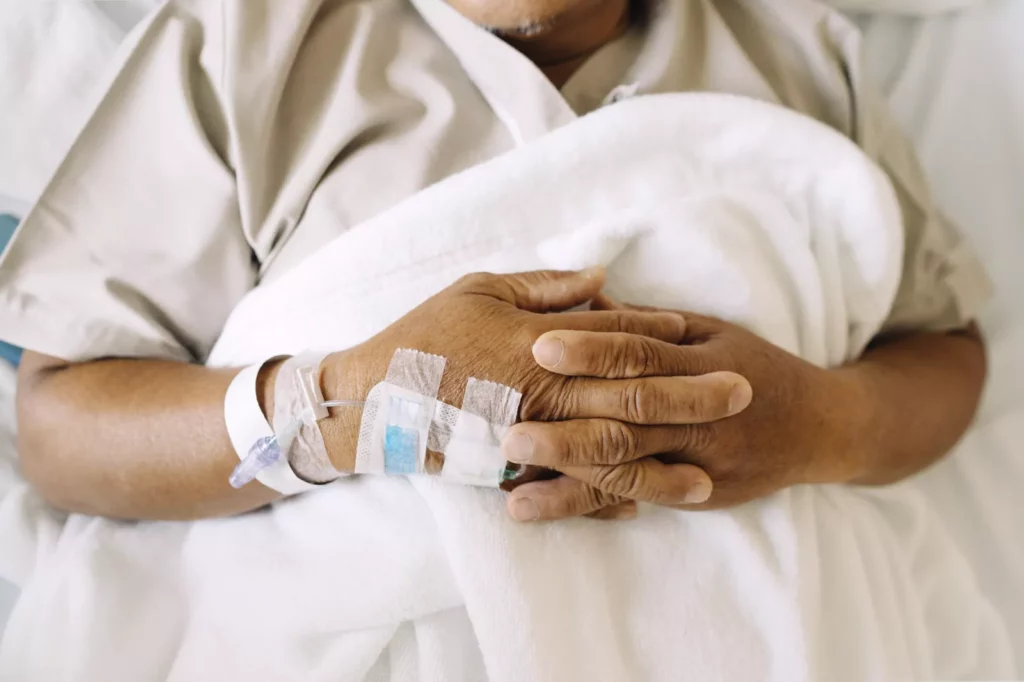
Patients are receiving life-altering diagnoses such as cancer, Parkinson’s disease and chronic kidney disease through the NHS app and over the telephone, leaving them to process the news without immediate access to a medical professional for support or explanation.
Campaigners have accused the health service of failing in its fundamental duty of care, urging that serious diagnoses should always be delivered in person. The growing reliance on digital communication means patients are increasingly left to piece together the implications of test results, scan reports and correspondence uploaded to their electronic records before any clinician has spoken to them.
‘Absolutely outrageous’: the patients who discovered their illness online
Steve, a patient from London, received his diagnosis of early-onset Parkinson’s disease in April 2023 after discovering the results on the NHS app’s test results page. He described the experience as “absolutely outrageous and frustrating,” saying he had been “let down by the NHS on numerous occasions.” When he sought further support, the health service informed him they were overwhelmed with Parkinson’s referrals and that he would have to “sit tight and wait.”
Another Parkinson’s patient, Dawn, learned of her condition four days after undergoing tests when she read correspondence between the hospital and her GP that had been uploaded to the app. She had no appointment with a neurologist scheduled for another 12 months, leaving her without specialist guidance following the life-changing discovery.
The problem extends to other serious conditions. Richard Carder, a 69-year-old retired police officer from Devon, discovered he had chronic kidney disease in June 2024 after checking his annual health check results on the app. Having heard nothing from his GP, he researched what his elevated creatinine levels indicated and concluded he likely had the condition, which involves irreparable kidney damage. He arranged a GP appointment for three weeks later but received a text message that Friday confirming the diagnosis, leaving him without professional support over the weekend.
“I did panic in some ways, which is why I went on to ‘Dr Google’. It was foolish but it was the only way I could get information,” he told The Telegraph. “I was reading the worst-case scenario and couldn’t actually ring a professional for help until Monday.”
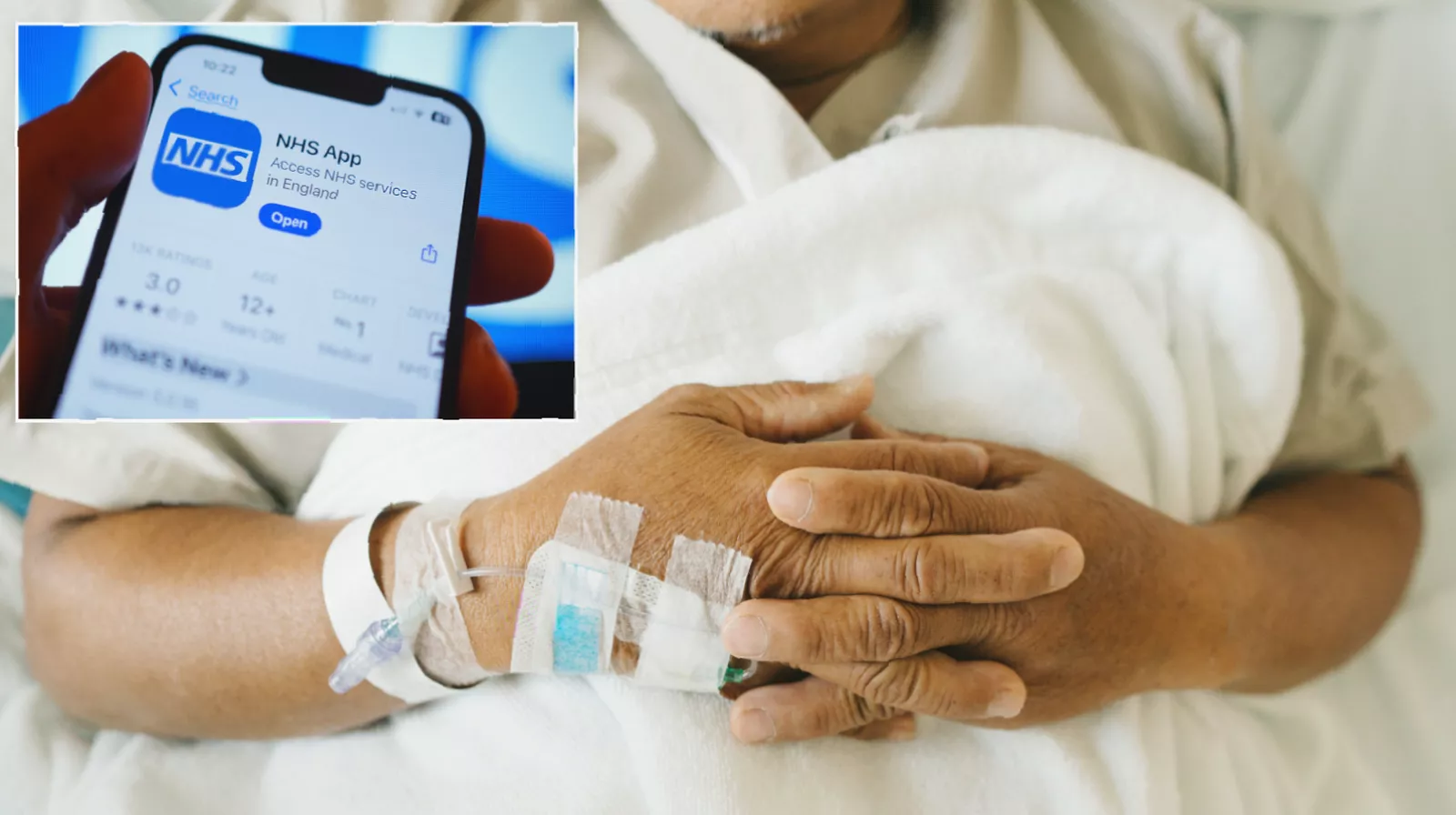
When Mr Carder contacted his GP surgery, the receptionist dismissed his concerns, telling him he should not worry because chronic kidney disease was common. “I said, ‘It might be to you, but it’s not to me.’ She was quite blasé and there was a little lack of compassion,” he recalled. He later questioned his GP about the timing of the text message, and the doctor acknowledged it “probably wasn’t the best thing to do.”
Two mothers separately told The Telegraph that they had learned through telephone calls that their children had been diagnosed with rare muscle-wasting conditions. Cancer patients have also reported discovering suspected diagnoses through the app before being contacted by a clinician. Cancer Research UK has noted that callers to its helpline sometimes need nurses to explain results visible in the app, with some having already pieced together the implications from clinical reports.
Data from Kidney Care UK’s report, Falling through the G-App, reveals that one in ten people discovered they had chronic kidney disease through the NHS app without prior awareness or discussion with a healthcare professional. Many patients did not have the opportunity to discuss their diagnosis and found it difficult to access necessary information, leading to dissatisfaction with their experience.
NHS guidance and calls for change
The NHS app, used by more than 13 million people as of September 2025, allows patients to view their health records, including consultations, test results and referral information. NHS England guidance states that positive test results, including cancer diagnoses, may be withheld from a patient’s record to allow clinicians time to contact them first. However, it also notes that patients may still see results before a clinician has made contact, and in such cases healthcare professionals should reach out as soon as possible.
In response to the growing number of patients receiving serious news through digital channels, NHS England has reissued guidance to local leaders making clear that procedures should be in place to ensure patients do not receive diagnoses for serious conditions through the app or other digital means without adequate support. The Royal College of Surgeons of Edinburgh has stressed that while the app is valuable, medical professionals should always be the ones to deliver a cancer diagnosis, providing the necessary skills and support.
An NHS spokesman said: “Sensitive results should always be delivered in person by a clinician, where patients can ask questions and be offered the right support. That’s why NHS England has recently reissued guidance to local leaders making clear procedures should be in place to ensure patients don’t receive diagnoses for serious conditions through digital channels like the NHS app.”

Following the Kidney Care UK report, NHS England leaders wrote to NHS Trusts and integrated care boards requesting immediate action to ensure patients receive diagnoses with appropriate support and context. A new programme, Diagnosis Connect, is due to launch in 2026 to connect patients diagnosed with long-term conditions to charities and support organisations via the NHS app.
Streeting’s ‘doctor in your pocket’ vision under scrutiny
These experiences reflect the consequences of Health Secretary Wes Streeting’s drive to digitise the health service, with his vision of a revamped NHS app functioning like a “doctor in your pocket.” However, diagnostic reports such as brain scans and cancer screenings are now being uploaded to patient records simultaneously with their transmission to consultants, often before any appointment can be arranged.
The broader NHS digital strategy aims to make digital a default, connecting services, empowering patients and improving outcomes through technology. A central part of this transformation is the move towards a Single Patient Record for each individual, accessible across all healthcare providers. Legislation is being introduced to mandate data sharing between GPs and hospitals to create these unified records, part of a £10 billion digitisation of the health service.
While some digital access advocates argue that withholding information can cause delays, the principle of providing human support alongside a serious diagnosis remains crucial. In the United States, the 21st Century Cures Act mandates immediate release of test results, with research showing high patient preference for early access. In Nordic countries such as Finland and Estonia, real-time results are released with high patient satisfaction reported.
The problem is partly attributed to GPs being responsible for uploading documents, sometimes without awareness of whether hospital staff have already communicated with the patient. The fragmentation of NHS systems and independent technology procurement processes also create inefficiencies and delays in deploying proven technologies. Concerns have been raised about safety risks for vulnerable individuals, such as domestic abuse survivors and stalking victims, who may not want their medical information readily accessible via the NHS app. Some have been advised to consider deleting the app or opting out of remote access until safety agreements are in place.