A 21-year-old student nurse was diagnosed with aggressive leukaemia at 19 after GPs initially suspected she had diabetes, and has described how her life was transformed in “the blink of an eye”.
Ayley Crawford, from Wishaw in North Lanarkshire, began experiencing constant sinus infections, colds and muscle weakness in March 2024. She also fainted during a university exam and developed a painful abscess under her arm, before struggling to eat or drink. Doctors referred her to University Hospital Wishaw for tests after finding high glucose levels that suggested diabetes.
On 23 May 2024, following further blood tests and hospital admissions, she was formally diagnosed with acute myeloid leukaemia (AML) — an aggressive blood cancer. She was immediately transferred to the Beatson Cancer Centre in Glasgow for treatment.
“My first thought was, ‘I’m going to die’,” Ms Crawford said. “I knew something was wrong with me, but I never thought it would turn out to be cancer.”
At the Beatson, she underwent four cycles of intravenous chemotherapy followed by chemotherapy in tablet form. She experienced nausea and hair loss, but said the care she received helped her remain in good spirits. “I kept thinking, I just need to get through this and then I’ll be able to get back to my life,” she added.

By November 2024, Ms Crawford was told she was in remission. She returned to part-time work, went on holiday and made plans to resume her nursing degree in September 2025.
But at a routine check-up in March 2025, doctors informed her that the cancer had returned — a relapse that she described as devastating. “I felt like everything I went through with my treatment had been for nothing,” she said. “I’d been saying to my family that I was feeling so well, it was a complete shock.”
Her doctors recommended a stem cell transplant. After searching registries, a suitable donor was found: an anonymous 21-year-old male from Australia. Ms Crawford’s AML was confirmed to have the NPM1-FLT3 mutation, a genetic profile that can influence prognosis and treatment decisions.
‘The worst thing I’ve ever endured’
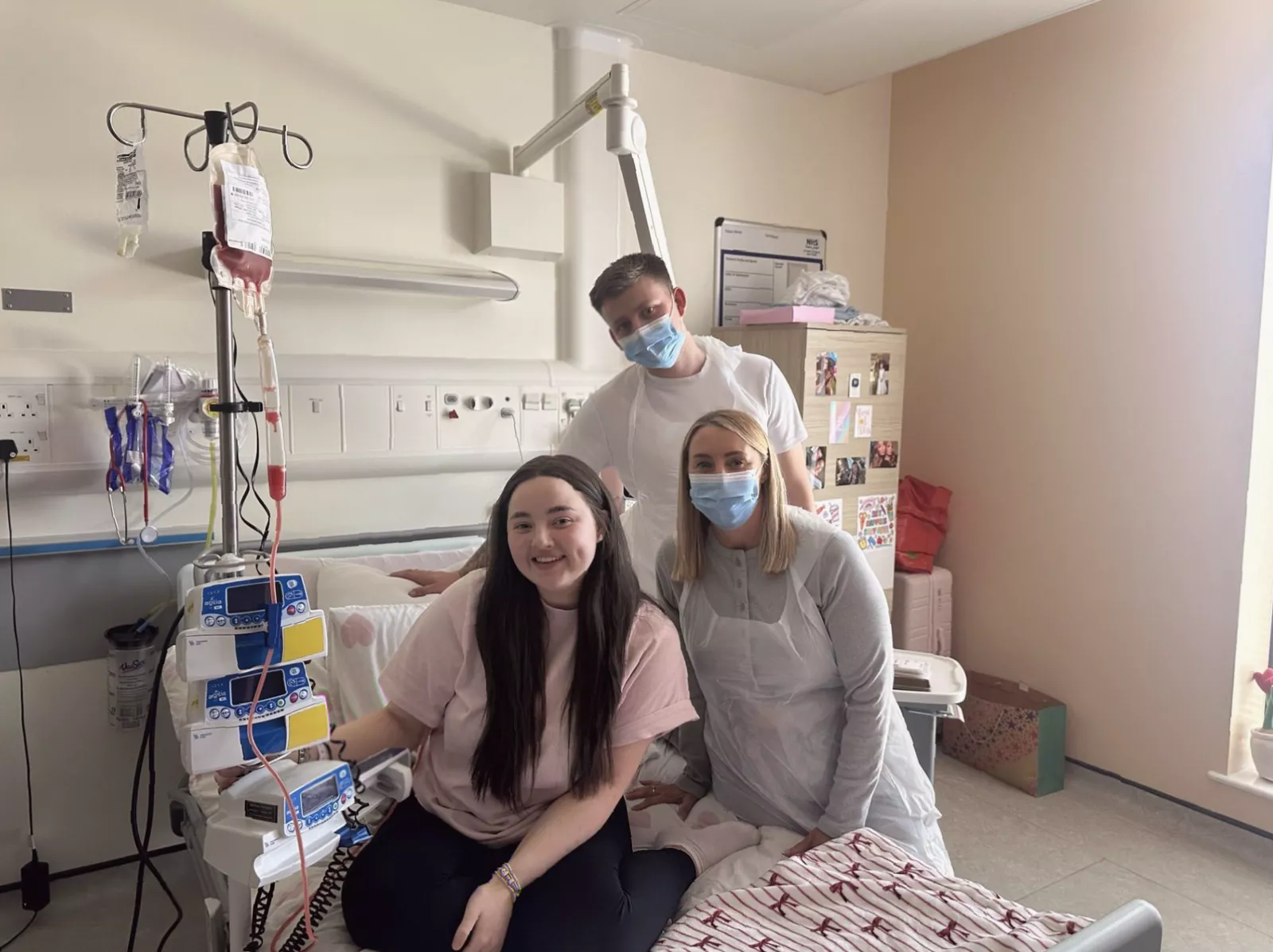
In July 2025 she was admitted to the Queen Elizabeth University Hospital (QEUH) in Glasgow for the transplant. Only a handful of visitors were allowed — her mother, her boyfriend Riley, and her friend Melissa. The isolation and physical toll were extreme.
“Going through transplant was honestly the worst thing I’ve ever endured,” Ms Crawford said. “I had ulcers in my digestive tract which led to significant weight loss. I wasn’t allowed out of my room for five weeks.”

After the procedure, she had to isolate for three months. She was put on a cocktail of medications, including an FLT3 inhibitor called Sorafenib, which caused a rash and swelling on her eyes. Her physical appearance deteriorated rapidly. “It was very hard for me dealing with how I looked as a young woman at the time,” she said.
Even basic movements became a struggle. “I was still so weak. Even walking from my bedroom to the bathroom next door felt too much,” she recalled. The loss of muscle mass has been a long recovery challenge, and she remains under close monitoring.
Despite the difficulties, she said the support of her family and friends was crucial. “I slowly started to recover and was able to celebrate Christmas 2025 which was so special.”
Ms Crawford is now once again in remission. She has made plans to travel this summer and will return to university in September 2026. Her experience has reshaped her career ambitions. “Every ward I was on, the nurses wanted me to come and join them once I was qualified. So I may actually go into oncology,” she said. “But my main aim right now is to get back to university and to catch up on all my missed time.”
She also noted that studying nursing helped her navigate the medical system. “I was really glad I was studying nursing as it made the medical terms so much easier and I could explain everything clearly to friends and family.”
Raising awareness of leukaemia signs
Fiona Hazell, chief executive of the research charity Leukaemia UK, praised Ms Crawford for sharing her story. “Many people aren’t aware of the signs and symptoms of leukaemia until they or someone they know is diagnosed,” she said.
According to Cancer Research UK data, more than 40% of people diagnosed with AML in England survive for at least one year, and more than 20% survive for five years or more — although the original article notes that 80% of patients do not survive beyond five years. Survival rates vary significantly by age and genetic factors. The charity Leukaemia UK runs the #SpotLeukaemia campaign to encourage the public to ask for a full blood count test if they experience unexplained symptoms.
A YouGov poll conducted in July 2024 for Leukaemia Care and Leukaemia UK found that only 14% of British adults could recognise the common signs of leukaemia, meaning 86% could not. World Leukemia Day is marked annually on 4 September to promote earlier diagnosis.
“Early diagnosis saves lives,” Ms Hazell said. “So we want to make sure more people are aware of the signs and symptoms, and to contact their GP to ask for a full blood count test if they’re experiencing them. Together, we can stop leukaemia from devastating so many lives.”

