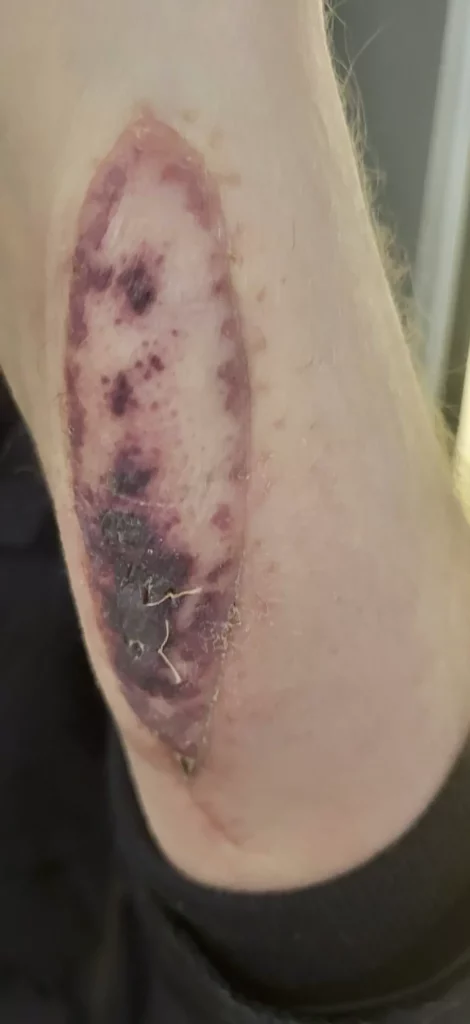
A patch of skin from an organ donor, grafted onto the forearm of a lung transplant patient, is being trialled in the UK as a revolutionary early warning system that could dramatically improve survival rates. Darren White, a 53-year-old former bus driver from Stockton-on-Tees, is among the first in the country to have the procedure, and credits it with protecting his new lung.
The Visible Warning
Three months after receiving a lung transplant in late 2024, Mr. White noticed a purple rash appearing on a small patch of skin on his arm. This was no ordinary rash; the skin had come from his lung donor. He sent photographs to his medical team, a biopsy was swiftly arranged, and it confirmed his body was beginning to reject the transplanted organ. “Anything that might help to avoid rejection was worth a try,” Mr. White said of his decision to join the trial.
The swift diagnosis allowed medics to treat him with steroids immediately. More than a year on, he is doing well and revels in the simple freedoms his transplant has restored. “I can be more of a dad,” he said, highlighting the joy of being able to take his three-year-old son, Daniel, to the park and push him on a swing.
The ‘Sentinel’ Science
Mr. White is a participant in the SENTINEL trial, a £2 million study led by the University of Oxford’s Surgical Intervention Trials Unit (SITU) in collaboration with NHS Blood and Transplant (NHSBT) and five UK transplant centres. The trial, which began in April 2024 and aims to recruit 152 patients, is funded by a partnership between the Medical Research Council (MRC) and the National Institute for Health and Care Research (NIHR).
The science hinges on the principle that skin acts as a more sensitive and visible “window” into the body’s immune response. Scientists believe skin rejects earlier and more observably than internal organs. A reaction on the so-called “sentinel skin flap” grafted to the arm can therefore raise an alarm before the transplanted lung itself is significantly damaged.
“The skin patch acts as a window into the body’s response to the transplant,” explained Professor Henk Giele, the trial’s chief investigator and Associate Professor of Plastic, Reconstructive, Transplant and Hand Surgery at the University of Oxford. Early detection enables quicker, more personalised treatment, which can help the organ function for longer and may allow for lower doses of powerful immunosuppressant drugs, which carry risks including cancer and diabetes.
If successful, the approach could cut lung transplant rejection rates by up to 50%, according to the trial team. Previous studies using similar sentinel skin grafts for intestinal transplants showed a reduction in rejection of approximately half.
Contrast with Current Challenges
The trial addresses a critical weakness in post-transplant care. Current methods for detecting lung rejection – including lung function tests, blood tests, and X-rays – can be difficult to interpret until rejection is advanced. The most definitive test, a lung biopsy, is invasive and carries risks such as pulmonary haemorrhage, pneumothorax, and even death.

Early symptoms like increasing shortness of breath, fatigue, or cough can also be subtle and mimic infections. “Rejection is a primary concern for transplant recipients,” said Emma Lawson, Organ Donation Innovation and Research Lead at NHSBT. This method offers a tangible, visual tool for proactive monitoring.
The concept is not entirely new; sentinel skin grafts have been used in studies for intestinal and pancreatic transplants with promise. Other research avenues for lung rejection include blood tests measuring donor DNA and ultrasound monitoring.
A Future Built on Consent and Hope
The pioneering trial relies on the generosity of donor families, who must give additional consent for the small skin graft to be taken. NHSBT specialist nurses facilitate these sensitive conversations. The lung transplants themselves are carried out by specialist Cardiothoracic Centre teams at Freeman Hospital, Harefield Hospital, Queen Elizabeth Hospital, Royal Papworth, and Wythenshawe Hospital.
The potential impact is significant against a sobering backdrop: around 55% of lung transplant patients are alive after five years, with chronic lung allograft dysfunction (CLAD) affecting half of all recipients and limiting average survival to about six years.
For patients, the psychological benefit of a visible monitoring system is profound. Helen Roper, who faces a potential lung transplant, finds the concept “extremely encouraging”. Adam Alderson, who received a skin graft during a multi-organ transplant in 2015, reported it helped identify rejection three times, leading to prompt treatment.
For Darren White, the proof is in his daily life, free from the shadow of undetected rejection. His experience offers a compelling glimpse into a future where transplant care is less reactive, less invasive, and more secure for the thousands of patients who depend on these life-saving procedures.