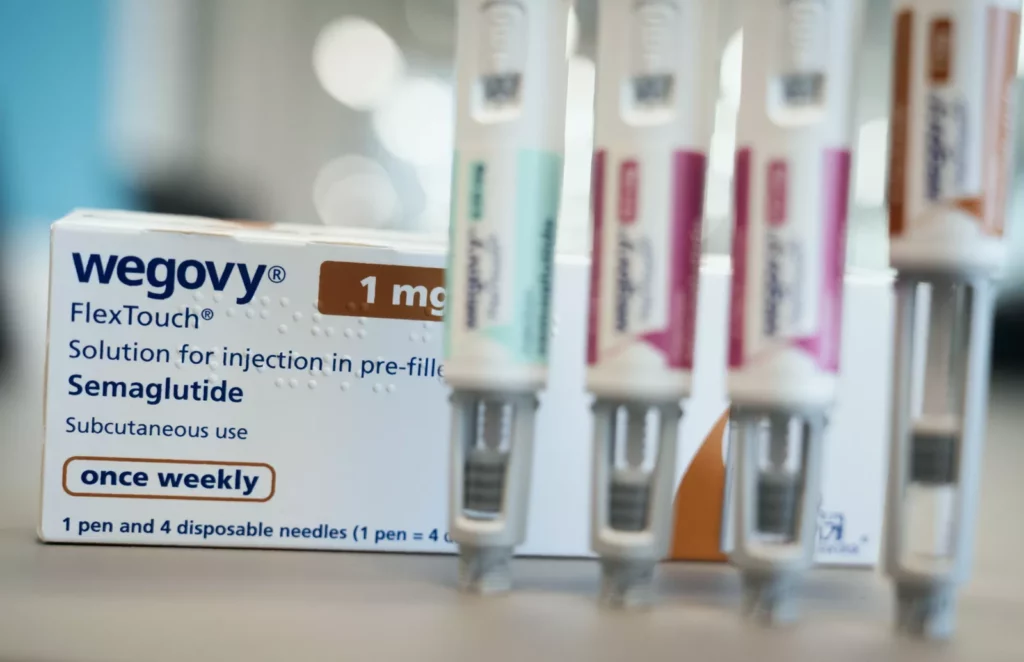
In a move set to reshape preventative heart care, a leading weight-loss medication has been formally approved for use within the NHS to cut the risk of deadly heart attacks and strokes. The decision transforms the drug from a tool for shedding pounds into a recognised guardian of cardiovascular health.
NICE green light for semaglutide
The NHS spending watchdog, the National Institute for Health and Care Excellence (Nice), has given the green light for semaglutide – sold under the brand name Wegovy – to be prescribed to overweight and obese patients who also live with established heart and circulatory conditions. The aim is specifically to reduce their risk of suffering a major cardiovascular event.
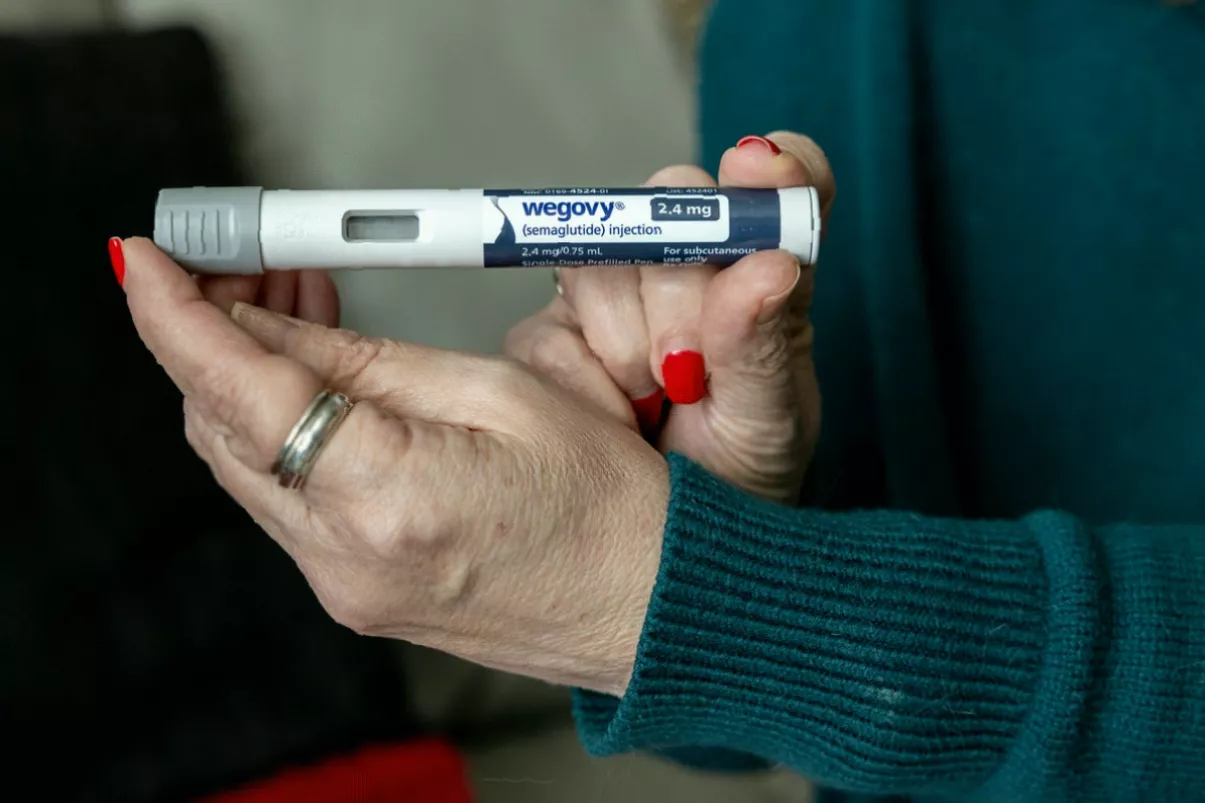
This means the injectable drug, which mimics a hormone called GLP-1 to regulate appetite and blood sugar, can now be officially offered in England and Wales both for weight management and for this new, crucial preventative purpose.
Experts hail a “major turning point”
Cardiometabolic specialists have welcomed the guidance as transformative. Naveed Sattar, professor of cardiometabolic medicine at the University of Glasgow, said the development represented a “major turning point in the battle against obesity”.
“We now have medicines that not only reduce heart attacks, strokes, and peripheral arterial disease, but also simultaneously lead to meaningful weight loss – which in turn lowers the risk of many weight-related conditions,” Professor Sattar said. He described the dual benefit as a “genuine win-win” that also improves quality of life, arguing that directly addressing a patient’s weight is now essential alongside managing blood pressure and cholesterol.
The critical need to protect muscle mass
While the benefits are significant, experts are issuing a clear and urgent warning about a key side effect that requires active management. They stress that GLP-1 receptor agonist drugs like semaglutide can reduce lean muscle mass as well as fat.
Robert Storey, professor of cardiology at the University of Sheffield, emphasised that prescribing “needs to be appropriately targeted”. “GLP-1 drugs can reduce muscle mass as well as fat so physical activity, such as resistance training, is important to counteract potential negative effects on muscle strength,” he said, noting this “may not be feasible in frail people.”
This point was strongly echoed by Huw Edwards, chief executive of the industry body ukactive. “While the impact of GLP-1 medications can be transformative, they are not a standalone solution,” he stated. “Evidence shows that without physical activity, particularly strength training, patients risk losing muscle mass, which can undermine long-term health outcomes. To ensure sustainable results for people taking these medications, treatment should be combined with structured physical activity and wider lifestyle support.”
Professor Storey added that the benefits of the drug must be “balanced against the risk of side effects” more broadly.

Implementation challenges and the “postcode lottery” risk
Beyond the clinical considerations, health leaders have pointed to significant practical hurdles in rolling out the treatment fairly. They have urged local integrated care boards (ICBs) to ensure consistent access and prevent a “postcode lottery” in care when the drugs become more widely available.
Riyaz Patel, professor of cardiology at UCL, highlighted the capacity challenge for the NHS. “We know, for example, that other highly beneficial drugs like inclisiran, for cholesterol lowering, have been variably delivered leading to significant postcode lotteries,” he said. “ICBs must ensure this does not happen with this Nice [guidance], else we risk exacerbating health inequalities, when if anything, this should be a powerful tool to reduce health inequality.”
Professor Storey also detailed the resource implications, noting that the “need for training people to inject the drug as well as ongoing monitoring and prescribing requires the allocation of NHS resources to ensure the benefits of this Nice guidance can be fully realised.”
Despite these challenges, Professor Patel concluded that the approval was “a really exciting development, for patients and doctors, giving us another powerful tool to reduce cardiovascular disease risk.”