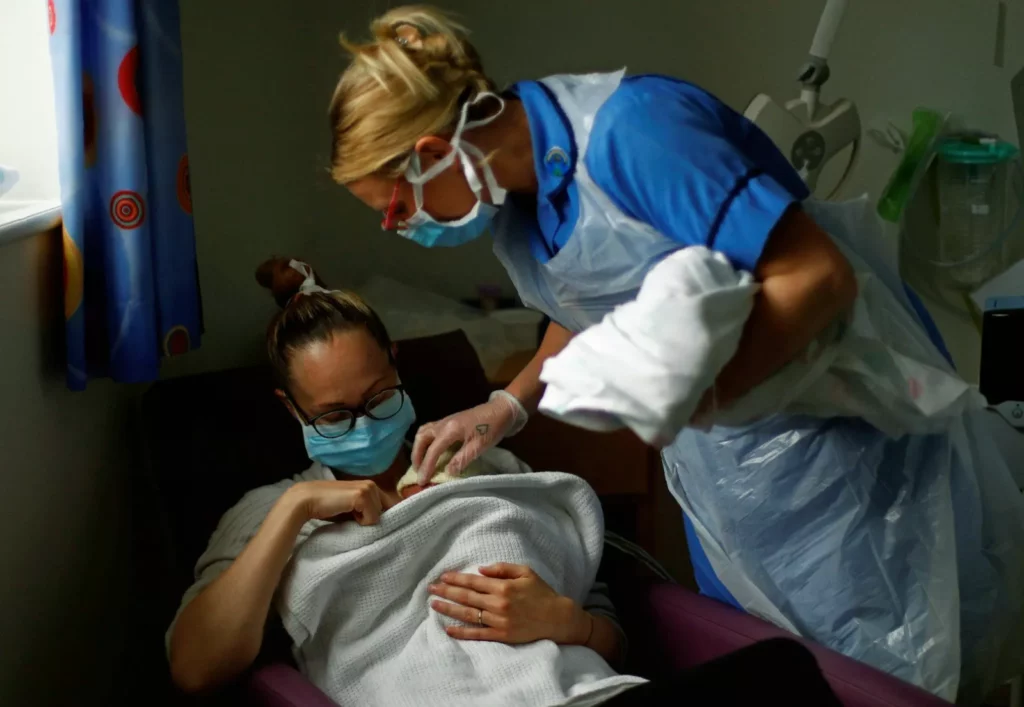
Maternity deaths in England have reached a 20-year high, with Black women now three times more likely to die during or after childbirth than white women, stark new figures reveal. The crisis has prompted the nursing and midwifery regulator to declare a “national emergency” and launch a fundamental overhaul of how midwives are trained.
New Anti-Racism Training for All Student Midwives
The Nursing and Midwifery Council (NMC), which approves all UK midwifery courses, is to integrate mandatory anti-racism training into university degrees from the next academic year. Paul Rees, the NMC’s Chief Executive and Registrar, stated that racism within maternity services “compounds the problem” and leads to “absolutely devastating consequences”.
All universities teaching midwifery must update their curriculum to include training on discrimination, racial biases, cultural curiosity, safety, and respect. The NMC said it will design a set of principles in the coming weeks, due for publication in late spring, with guidance from Black, Asian and other ethnic minority women who have experienced poor maternity care. A similar set of principles will be developed for nursing programmes.
The Scale of the Crisis: Mortality and Systemic Failure
The push for new training follows years of escalating concern. The NHS has received 22 safety warnings from official bodies about discrimination in maternity wards over the past decade, yet the situation has worsened. Reviews into maternal and baby deaths, as well as major maternity scandals, have repeatedly pointed to racism as a contributing factor in avoidable tragedies.
Data from MBRRACE-UK, which audits maternal deaths, indicates a nearly three-fold difference in mortality rates for women from Black ethnic backgrounds compared to white women. Black babies are twice as likely to be stillborn. Asian women also face increased risks, with higher mortality rates than white women. Furthermore, women living in the most deprived areas are more than twice as likely to die compared to those in the least affluent areas.

An independent investigation into NHS maternity and neonatal services, chaired by Baroness Valerie Amos, has been a significant catalyst. Its interim report, published in February 2026, found services under severe strain and “unacceptable care” leading to “tragic consequences”. It highlighted staff shortages, poor leadership, a lack of accountability, and persistent racism and discrimination contributing to worse outcomes for Black, Asian and disadvantaged women.
Specific Discrimination and Its Devastating Impact
The discrimination faced by women is not abstract but manifests in specific, harmful interactions during critical moments of care. Testimonies gathered by investigations reveal a pattern of dangerous stereotyping and neglect.
Black mothers have reported being denied pain relief by midwives who labelled them “tough” or “demanding”, with some told they were better at enduring childbirth due to having “tough skin”. Others have been stereotyped as angry or aggressive when raising concerns. Asian women, meanwhile, have been dismissively stereotyped as ‘princesses’, with staff heard making comments like, “The bloody Asian ones just go on and on and on.”
Muslim families have reported feeling discriminated against based on their religion, while failures to provide translation services have had catastrophic results. In one instance, a family only learned of their baby’s death when they overheard staff talking, having been denied an interpreter.
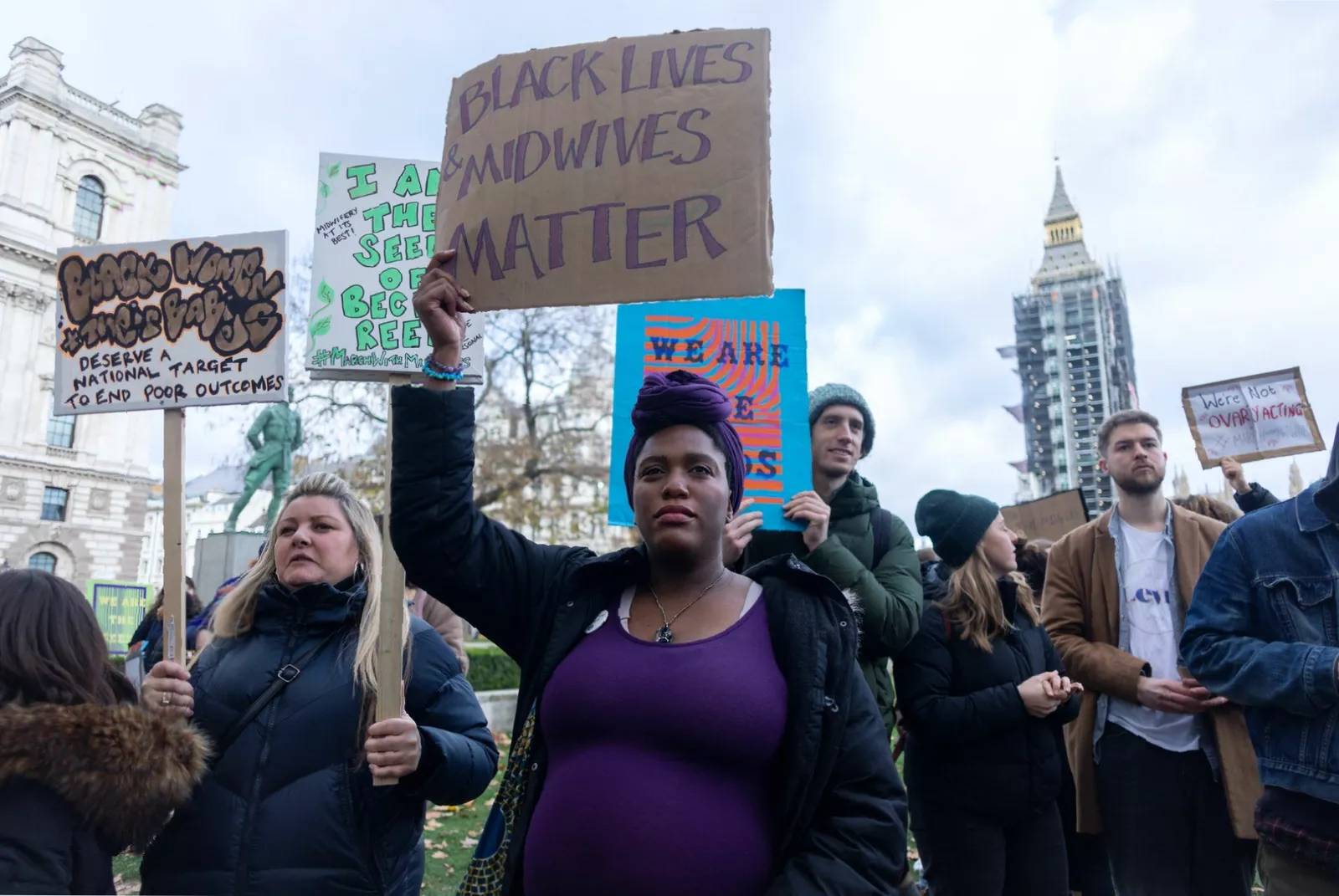
This erosion of trust has profound consequences. Some Black women report feeling so unsafe they consider leaving the UK to give birth. The awareness of the mortality statistics itself generates fear, stress, and anxiety during pregnancy, with mental health issues being a leading cause of maternal deaths. Campaigners and the Royal College of Midwives argue that addressing these deep-seated issues requires mandatory cultural competency training for all practising midwives, not just student midwives and leaders.
Government Response and Ongoing Criticism
Sharon Hodgson MP, the Public Health Minister, welcomed the NMC’s move, stating the government is taking “urgent action” to tackle disparities it calls “unacceptable”. The Department for Health and Social Care highlighted an anti-discrimination programme, hiring more midwives, and a new Maternity Taskforce chaired by the Health Secretary to deliver rapid improvements.
However, the government has rejected calls from MPs for mandatory cultural competency training for all practising midwives, stating it is part of a core competency framework that currently only applies to leaders and consultants. This stance has drawn criticism, particularly alongside figures showing the NHS in England has paid out £27.4 billion in maternity negligence claims since 2019, a sum attributed to systemic failings.
The scale of the challenge is underscored by a significant midwife shortfall of over 2,500 in England and existing gaps in understanding. A study noted that while student midwives see the value of anti-racism training, access is limited and comprehension of cultural competency is only “somewhat” understood. As the NMC works to reform training from the ground up, the pressure remains to ensure existing staff and systems can change quickly enough to address what all parties now label an emergency.