Amy Bamford, 35, lives with what she has been told is an ‘unfixable’ hernia, a permanent physical reminder of a catastrophic medical ordeal that began with routine surgery and ended with her body forever changed.
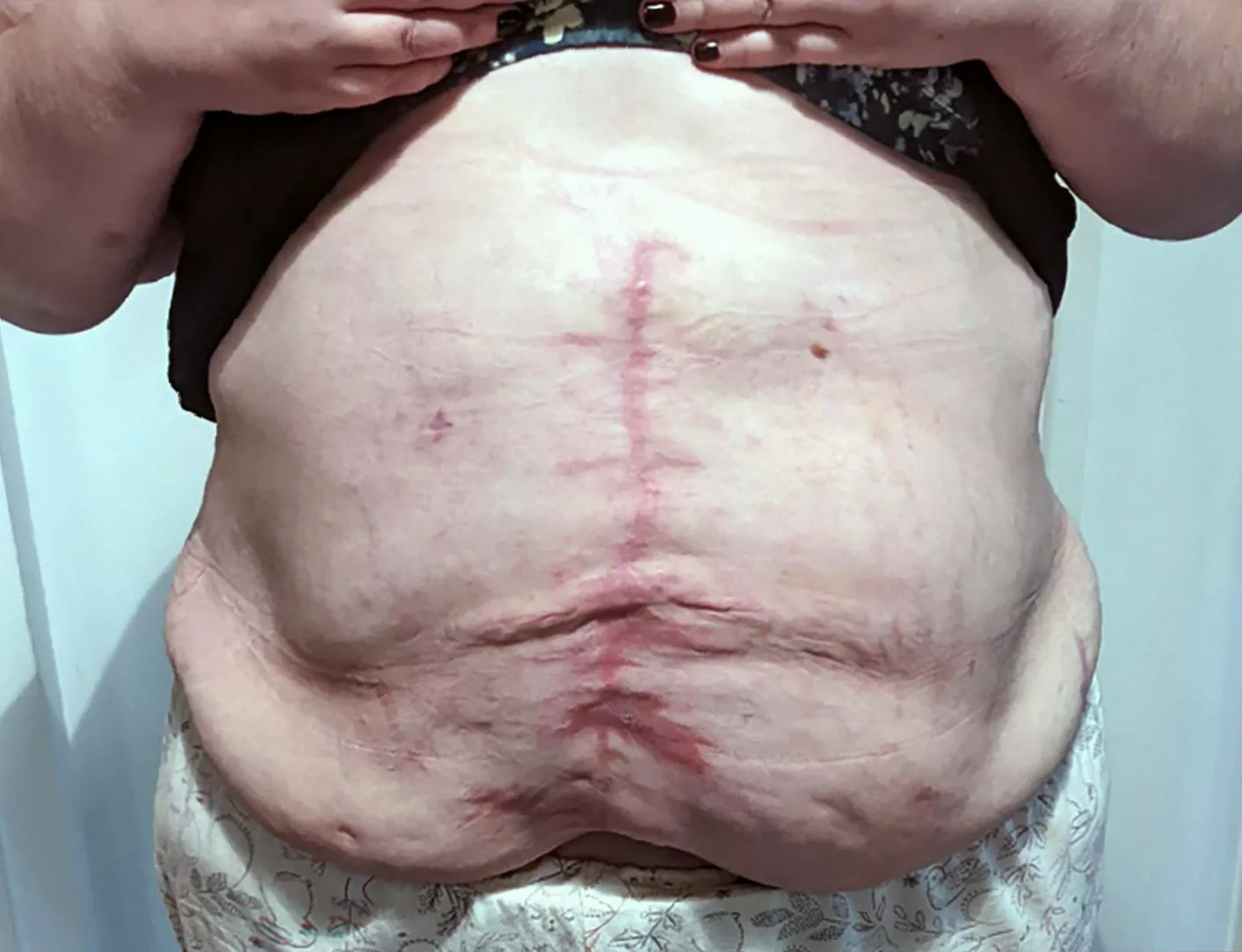
The incisional hernia in her abdomen, which began developing in August 2022, protrudes through a 25-centimetre gap in her abdominal wall. Surgeons and doctors, following both NHS and private consultations, have advised her against attempting repair. For Amy, from Chesterfield, this means learning to live with a large, visible bulge that is stable but persistently uncomfortable, and which represents a complex intersection of surgical trauma, missed opportunities, and ultimate clinical judgment.
A cascade of complications
Amy’s path to this point began with surgery for lipoedema, a painful condition involving abnormal fat accumulation. After five such procedures, a severe complication arose. Following her fifth operation, she developed abdominal sepsis, a life-threatening response to infection that can cause severe tissue damage and muscle wasting.
To save her life, surgeons performed eight emergency operations within a single month to clear infected tissue. During this intense period, 80 centimetres of her small intestine was removed. The trauma of being cut from the top to the bottom of her abdomen, compounded by the physiological impact of sepsis, critically weakened her abdominal muscle wall. This damage created the perfect conditions for a hernia to later develop.

In the years that followed, Amy was a frequent visitor to hospital and her GP. “I was constantly telling different medical professionals about my abdominal surgeries, the concern about my growing stomach,” she explains. However, she states that no one saw it as a pressing concern urgent enough to accelerate a referral, nor did anyone warn her that such hernias can reach a point of being inoperable.
Why surgery is now deemed too risky
The medical reasoning behind the decision not to operate is multifaceted and steeped in sober risk assessment. Amy has what is classified as a ‘giant’ incisional hernia, a type that occurs at the site of a previous surgical scar and is reported to develop in 10-20% of patients after abdominal surgery.
While incisional hernias do not heal without surgery and typically require repair to prevent future emergencies like strangulation—where blood supply is cut off—the procedure is highly complex. Recurrence rates for incisional hernias are significant, ranging from 23% to 50% according to surgical studies.

For Amy, the risks are compounded exponentially by her unique medical history. “I have to add on my complex medical history, I’ve had a stroke, there’s a lot of damage in my abdomen, so I’m at a higher risk of complications,” she says. The potential complications of such major surgery include severe bleeding, infection, injury to internal organs, and, given the extensive prior damage, a high likelihood of the hernia simply recurring. In her case, clinicians have concluded that the dangers of attempting a repair outweigh the benefits, as the hernia is currently stable and not at risk of strangulation.
The broader context of healthcare access also shadows her story. While private hernia repair in the UK can cost between approximately £2,200 and over £6,000 plus consultation fees, the NHS, which she has consulted, operates under significant strain. The NHS constitutional standard is an 18-week maximum wait for non-urgent treatment, but a backlog means millions wait longer. Amy’s experience of delayed recognition and referral occurred within this pressured system.
Learning to live with the unfixable
Coming to terms with this reality has been a profound emotional challenge. The physical presence of the hernia carries a heavy psychological toll, affecting body image and self-esteem. “I flit between hating my body and being grateful for what my body has been through and recovered from,” Amy admits. Mental health difficulties, including anxiety and depression, are commonly reported by those living with such visible abdominal conditions.
She has found steadfast support in her husband, saying the journey has brought them “closer together.” To forge a sense of agency and community, she now runs an Instagram account, @hernia_troll_uk, to raise awareness of her experience. The platform has brought hate comments, but Amy has developed resilience. “I don’t need to be validated by random people online,” she states, using keyword blocks to protect her followers and choosing to engage, laugh, or ignore the negativity as she sees fit.
Her story is a stark illustration of how a single surgical complication can irrevocably alter a life, and how medical decisions must sometimes balance the desire to fix against the imperative to first do no harm. For Amy Bamford, the path forward is not one of cure, but of daily management and hard-won acceptance.

