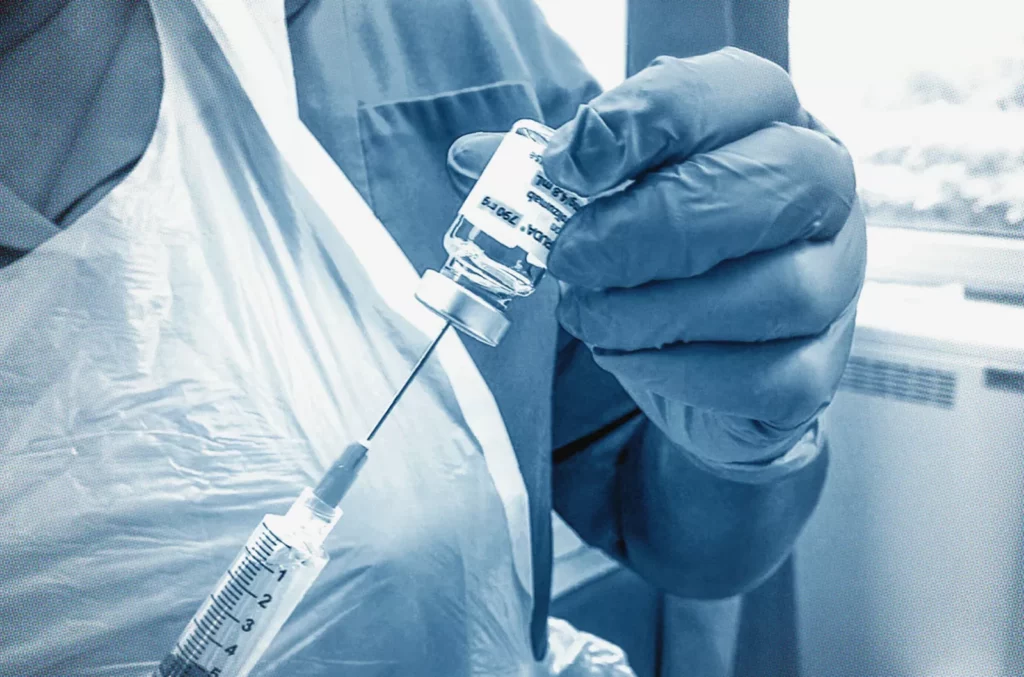
Cancer nurses across the UK are being exposed to hazardous chemotherapy drugs without adequate protective equipment, putting them at increased risk of miscarriage, infertility and other serious health conditions, an investigation has found.
Tens of thousands of NHS healthcare workers administer toxic medicines for cancer, rheumatoid arthritis, HIV and multiple sclerosis, yet most are routinely provided with only a plastic apron and gloves as protection. Without proper personal protective equipment (PPE), staff can inhale hazardous particles or absorb liquids through the skin, and can come into contact with contaminated surfaces or spills.
The risks are well documented. In September last year, the NHS West Midlands Cancer Alliance published guidance warning that “inadequate control measures” could cause miscarriage, birth defects, liver damage, abnormal cell formations, abdominal pain, nasal sores and vomiting. Multiple studies have linked exposure to these drugs with infertility among healthcare workers. A prospective study of nurses in the United States and Canada found a “suggestive positive association” between handling antineoplastic drugs and miscarriage, particularly among those who did not consistently use PPE and engineering controls.
Despite this evidence, the UK lags behind other countries. In the United States, the Centres for Disease Control and Prevention issued an alert over the risks, and staff are routinely given full surgical gowns, masks and double gloves. The US also follows USP guidelines, which mandate full PPE for all areas handling hazardous drugs. The European Union strengthened its requirements through Directive (EU) 2022/431. In Britain, however, guidelines allow NHS trusts to provide the “bare minimum”.
Health risks and the gap in protection
The UK’s Control of Substances Hazardous to Health (COSHH) Regulations 2002 require employers to assess risks and implement adequate controls. For carcinogens and mutagens, exposure must be kept “as low as is reasonably practicable” (ALARP). Crucially, COSHH does not mandate the same level of control for reproductive toxins as for carcinogens or mutagens. There is no specific UK legislation or guidance for hazardous medicinal products (HMPs) beyond the general COSHH framework.
Professor Karen Campbell, a former president of the UK Oncology Nurse Society (UKONS) and a cancer nurse for 30 years, published a study last year that laid bare the scale of the problem. Of 747 nurses surveyed, 97 per cent said they were primarily given only plastic aprons when administering cancer drugs. Just 62 per cent received the correct gloves labelled for use in chemotherapy; 53 per cent were given general-purpose gloves. Only 44 per cent of staff said they consistently used “closed system transfer devices” – mechanically sealed, leak-proof containers that cut the risk of exposure during preparation and administration of chemotherapy drugs.
Professor Campbell described this level of protection as “inadequate”. Among the nurses who responded, 161 reported health impacts including headaches, hair loss, fatigue, skin irritation, nausea, dizziness and miscarriage. The research briefing notes that a Cochrane review commissioned by UKONS concluded the use of closed systems in administration could neither be supported nor refuted, based on studies mostly conducted in pharmacy areas rather than clinical settings. Studies have also found that work surfaces where cytostatic drugs are handled are often contaminated, and that packaging from wholesalers can carry residue, meaning gloves are needed even during unpacking.
Nurse testimonies reveal the personal toll
Alison Simons, a cancer nurse with more than two decades of experience, believes her three miscarriages may be linked to working without adequate protection. Starting her career in the mid-1990s, she recalled: “When I was giving chemo, all we wore were plastic aprons and gloves to our wrists. I experienced three miscarriages, and at first, I didn’t make any link between giving chemotherapy at all. In fact, it was my GP who said you give chemotherapy, don’t you? When I started talking to colleagues, they were also experiencing similar things, such as miscarriages and fertility issues.”
Ms Simons, now a senior lecturer in applied cancer practice and a doctoral student at Birmingham City University, said many trusts still fail to implement known safety measures. “It’s particularly frustrating because we know there are things out there to protect us, and they’re not being used. It does beg the question, are we not worth it?”
Samantha Toland, a nurse consultant in cancer care for 26 years and lead cancer therapy nurse at Worcestershire Acute Hospitals Trust, echoed the concern. “I, too, experienced a miscarriage in between my two children, but didn’t think anything of it… It was more when I started teaching; we both concluded that this was bigger than we thought it was.” She said her current trust is very good on the matter, but in previous workplaces controls were lacking. “I’ve had colleagues who have had multiple miscarriages, up to six or seven, and had to be off work for most of their pregnancy. The concern is that nurses are not getting the level of protection they should have… there’s that feeling when you know there are things that could help, and nobody seems to be putting those into place.”
Professor Campbell said the risks have been known for decades but are more visible now because of the growing number of people undergoing cancer treatment. She warned that the workforce is often young and female, and may not have a strong voice. “I think it’s probably a very big can of worms to open up… My main fear is that the workforce is quite young, it’s women, and they don’t have much of a voice. You [ministers] have to protect your workers, [or] ultimately you won’t have anybody working in the NHS… why would you let them suffer?”
Calls for stronger regulation
The Royal College of Nursing is calling on the Health and Safety Executive (HSE) and the government to implement minimum standards for the control of hazardous medicines. Current regulations require employers to ensure exposure is “as low as reasonably practicable”, but the RCN argues the wording is subjective and has led to variations in how hospitals implement protections. It wants the requirement changed to “the lowest possible level”, which would compel stronger employer controls.
Louise Church, health, safety and wellbeing senior national officer for the RCN, said: “The RCN recognises that these are vital treatments for patients, but what we want to see is that nurses and staff are properly protected when they are handling and caring for patients using these substances.”
Labour MP Luke Akhurst, who received chemotherapy himself in 2009 and has raised the issue with ministers, said the government had a duty to protect workers. “This is about the NHS staff who are there for when you are really acutely ill, these are the people who are saving your life through cancer treatment, and none of us who have been for life-threatening illness would ever want the staff who are helping us to have their health damaged. [Ministers and the NHS] have a moral responsibility, the safety of workers, that’s what we’re about as a Labour government, but particularly people who are working on such an important task as saving people’s lives.”
An NHS spokesperson said: “The safety of NHS staff is paramount, and NHS trusts have a duty in law to protect staff from being exposed to hazardous medicinal products – with clear regulations and guidance in place on the handling of these substances.” The HSE, the Department for Work and Pensions, which oversees health and safety at work laws, and the Department of Health and Social Care have been approached for comment.
Broader failures in NHS PPE procurement
The issue extends beyond cancer wards. In a separate but related case, NHS laboratory staff have been exposed to dangerously high levels of formaldehyde, a chemical linked to cancers and damage to the respiratory, female reproductive and nervous systems. Some staff have been left disabled or forced to leave their jobs due to occupational asthma linked to formaldehyde exposure. The UK’s legal limit for workplace exposure to formaldehyde is 2 parts per million over eight hours – seven times higher than the EU limit and the highest in the world. The HSE has stated that lowering the limit would not provide a health risk benefit because the legal requirement is already to reduce exposure to the lowest reasonably practicable level.
Meanwhile, investigations have revealed broader problems with PPE procurement. The UK government has sourced medical gloves from manufacturers such as Top Glove, which has faced multiple allegations of worker exploitation and “slave-like conditions”. Despite US import bans on Top Glove PPE due to these allegations, the company’s gloves have been supplied to NHS hospitals. Similar concerns have been raised about Supermax, another glove manufacturer accused of labour abuses. In a separate case, a High Court judge ruled that PPE Medpro, a company linked to Baroness Michelle Mone, supplied defective PPE for the NHS, and the Department of Health and Social Care was ordered to recover £122 million paid for sterile surgical gowns that did not meet specifications.