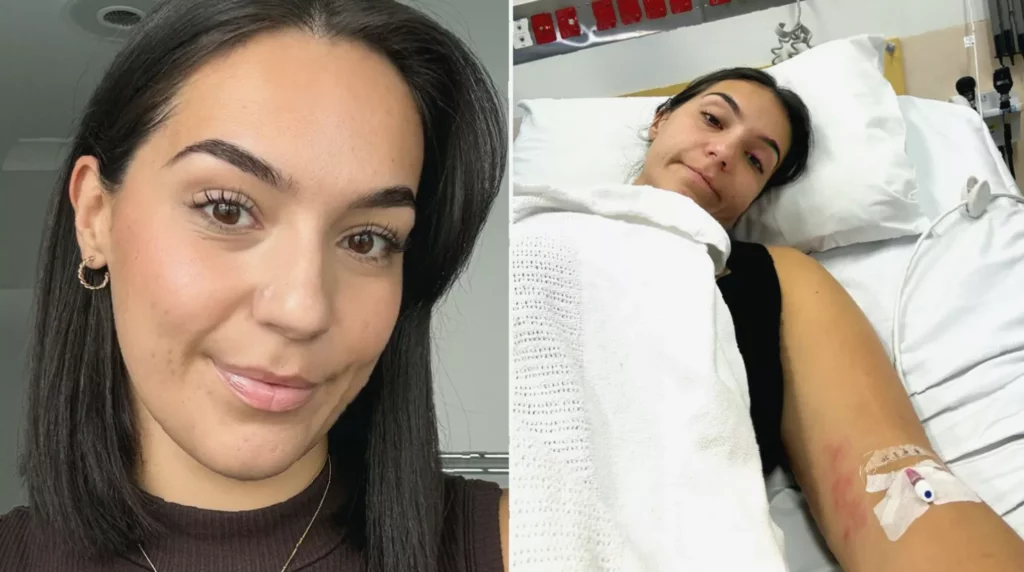
For nearly a year, 26-year-old Sumbul Ari knew something was profoundly wrong with her body. What began as relentless itching in April 2025 escalated to a point where she would scratch herself with sharp objects until she bled, waking to find blood on her sheets. She suffered extreme fatigue, intense night sweats, and fluctuating body temperatures. Yet, each time she sought help from her GP in Cairns, Queensland, she was told there was nothing seriously amiss.
‘I was dismissed again and again’
Her desperate search for answers saw her concerns repeatedly minimised. The first doctor she consulted about the itching advised her to moisturise, attributing it to the hot, humid climate. A second diagnosed a yeast infection. Subsequent visits led to diagnoses of scabies and eczema. “I knew deep down it wasn’t a skin issue, it felt systemic,” Sumbul says. Blood and stool tests returned as largely normal, showing only borderline anaemia, and she was dismissed once more.
The impact of being consistently unheard by medical professionals became a torturous ordeal in itself. In desperation, she turned to alternative treatments, spending money on a parasite cleanse and visiting a naturopath. While a herbal treatment provided a fleeting three-week respite, the itching returned worse than before. After being advised to see a skin specialist, she says she “gave up on the medical system.” Her experience underscores a documented issue in Australia, where lymphomas are among the cancers most commonly misdiagnosed, sometimes with severe consequences.

The lump that changed everything
The turning point came when Sumbul discovered a lump on her neck. A frantic internet search suggested lymphoma. Reading the symptoms—persistent itching, drenching night sweats, unexplained fever, and fatigue—was a chilling moment of recognition. “I just thought, ‘Oh my gosh, I think I have cancer,'” she recalls.
The next day, she pleaded with a doctor to take her seriously. This time, she was examined properly. Multiple swollen lymph nodes were found, triggering an urgent referral for an ultrasound. Within hours, her life altered completely. The scan revealed abnormal and enlarged lymph nodes, sending her straight to the emergency department. Further tests showed lymph nodes on her chest, neck, and spleen. A biopsy, PET scan, and heart scan followed. On March 17, 2026, almost a year after her symptoms began, Sumbul was diagnosed with Stage 2-3 Hodgkin’s lymphoma.
These symptoms—the severe itching (pruritus), night sweats, fatigue, and later the swollen lymph nodes—are all recognised indicators of Hodgkin’s lymphoma. The disease often presents with painless lumps in the neck, armpit, or groin, and so-called “B symptoms” like fevers, weight loss, and drenching sweats can indicate its stage and progression.
Relief, anger, and the path to treatment
Her initial reaction to the diagnosis was not fear, but profound relief. “I didn’t have to itch myself to death anymore,” she says. The validation was immediate; after her first chemotherapy session, the relentless itching stopped entirely, allowing her a full night’s rest for the first time in months.
That relief, however, was quickly accompanied by anger. The 11-month delay meant her cancer had progressed to an advanced stage before treatment could begin. Medical research indicates that such delays can lead to disease progression, necessitate more aggressive treatment, and impact survival rates. For Sumbul, it meant confronting a Stage 2-3 diagnosis, which typically requires intensive chemotherapy. Treatment for this stage often involves 4 to 6 cycles, with radiotherapy sometimes used afterwards.
The prognosis for Hodgkin’s lymphoma is generally positive, with cure rates between 80% and 95%, and a five-year survival rate in Australia of 79% for all lymphomas. However, early detection significantly improves outcomes. Sumbul’s journey highlights the tangible cost of a delayed diagnosis: a more intensive treatment road than might otherwise have been necessary.

Looking ahead, Sumbul is focusing on recovery and future goals, including her ambition to complete a full Ironman before she turns 30. Her story has unfolded against a national backdrop where an estimated 7,759 new cases of lymphoma were expected to be diagnosed in Australia in 2025. For others in similar situations, organisations like Cancer Council Australia, Lymphoma Australia, and the Leukaemia Foundation offer support and information.
For Sumbul, the psychological scars of being dismissed linger as deeply as the physical ones. She describes the feeling of being unheard as the “worst feeling,” a sentiment that resonates with many patients who face similar battles within healthcare systems. Her path forward is now clear, but the months of misdiagnosis have left an indelible mark.