For months, Louise Rossiter’s GP told her the pain under her ribs was simply acid reflux. By the time she reached A&E with yellowing eyes and was diagnosed with cholangiocarcinoma, or bile duct cancer, the opportunity for an easier fight had long passed.
Her story, moving from initial dismissal through surgery and recurrence to palliative care, exposes critical gaps in the UK’s awareness and treatment of a cancer that is becoming less rare by the day. “I felt devastated for not knowing anything,” she says. “But I was cross, too – at my GP for not spotting the signs but also at the general lack of awareness.”
A Disease That Does Not Discriminate
Cholangiocarcinoma is a cancer of the bile ducts, the tubes connecting the liver to the gut. Once considered obscure, its incidence has more than doubled in the UK over the past two decades. According to the UK’s only dedicated charity, AMMF, cases in England rose from 1,165 in 2001 to 2,635 in 2019.
Contrary to outdated assumptions that it only affects older men, this cancer does not discriminate. Data shows it occurs almost equally in men and women, with over 20% of patients in England diagnosed under the age of 65. AMMF reports a noticeable rise in cases among younger adults, particularly women aged 20 to 40.
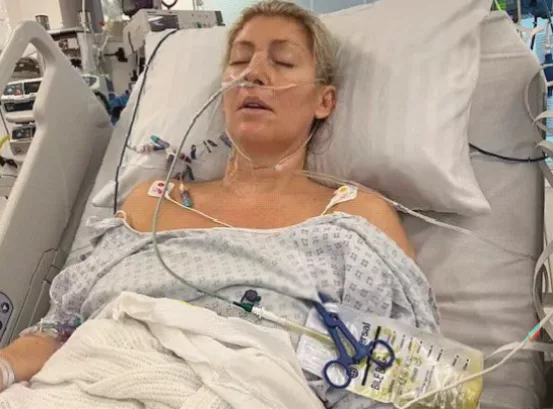
The disease is notoriously stealthy. Early symptoms are non-specific—fatigue, weight loss, vague discomfort—and easily mistaken for conditions like gallstones or, as in Louise’s case, acid reflux. It is often only when a tumour blocks the bile duct, causing the classic signs of jaundice (yellowing of the eyes and skin), dark urine, and pale stools, that the alarm is raised. By then, it is frequently advanced. Nearly half of all cholangiocarcinoma diagnoses in England are made via emergency presentation.
The Treatment Chasm
Louise’s journey reflects the standard, yet severely limited, treatment pathway. After an ERCP procedure inserted a stent to relieve the blockage, she underwent a liver resection in July 2022—surgery being the only potentially curative option. “I felt brand new,” she said after the stent, but the battle was far from over.
Despite follow-up chemotherapy and being declared cancer-free, her disease returned within months, scattered across her liver and inoperable. A further blow came with the discovery of a rare gene mutation, rendering standard chemotherapy and many NHS-approved targeted therapies ineffective for her. “My only hope was targeted therapy,” she explains, “I then learned I have a very rare gene mutation, meaning I won’t respond.”

This points to a broader crisis in care. Survival rates for cholangiocarcinoma are among the worst of any cancer, with a five-year survival rate in England historically around just 5%. AMMF states that more than half of NHS patients diagnosed with the disease do not receive any active treatment at all. Furthermore, mortality rates are almost 40% higher in the most socioeconomically deprived groups compared to the least deprived.
For patients like Louise, the disparity in global treatment access is a source of acute frustration. On international patient forums, she sees counterparts in America and Australia accessing advanced treatments not yet available in the UK. “For patients like me, this simply isn’t good enough,” she says.
Campaigning for a ‘Fairer Deal, Faster’
Now on palliative care but refusing to give up, Louise has channeled her energy into advocacy. She is working with AMMF’s ‘Rethink Liver Cancer’ campaign, alongside fashion designer Dame Zandra Rhodes—a fellow survivor—and photographer Rankin.

The campaign’s goal, encapsulated in the slogan ‘A Fairer Deal, Faster’, is to push for earlier diagnosis, equitable access to specialists and treatments, and increased research funding. Key to this is improving molecular testing to match patients with emerging targeted therapies and ensuring all patients see a specialist surgeon experienced in biliary cancers.
Louise will take this message directly to policymakers, attending a reception for MPs and NHS leaders at the House of Commons. “It’s high time that this cancer got the attention, funding and research that other cancers do,” she asserts. “It’s time the UK caught up with the rest of the world.”
Her fight, from a misdiagnosed pain under the rib to a national campaign, underscores a brutal truth: for thousands in the UK, the odds remain stacked against a disease that is rising in prevalence but languishing in priority.

