Venous leg ulcers have doubled in prevalence over the past decade, leaving an estimated half a million people across the United Kingdom living with the largely unrecognised condition. The chronic wounds, caused by poor blood circulation in the veins, are placing a mounting burden on patients and the NHS, costing the health service an estimated £2.7 billion annually.
Prevalence and Demographics
Venous leg ulcers are the most common type of leg ulcer, accounting for more than 60% of all cases. While they affect roughly one in 500 people in the UK, the rate rises sharply with age: approximately one in 50 people over 80 have the condition. Lifetime incidence of venous leg ulceration in the UK is around 1%, with a point prevalence of one to four per 1,000 of the general population. That figure climbs to 25 per 1,000 for those over 85. Globally, up to 3% of the adult population is affected. There is a notable sex bias: the female-to-male ratio is generally 2:1, although in patients under 40, men are more predominantly affected.
The financial toll is substantial. The total annual cost of wound management in the UK was estimated at £8.3 billion in 2017/18, with £5.6 billion attributed to unhealed wounds. Venous leg ulcers alone contribute an estimated £941 million annually, with community nursing care representing the largest portion of these costs. Sub-optimal care can cost up to ten times more than correctly managed treatment.
Causes and Symptoms
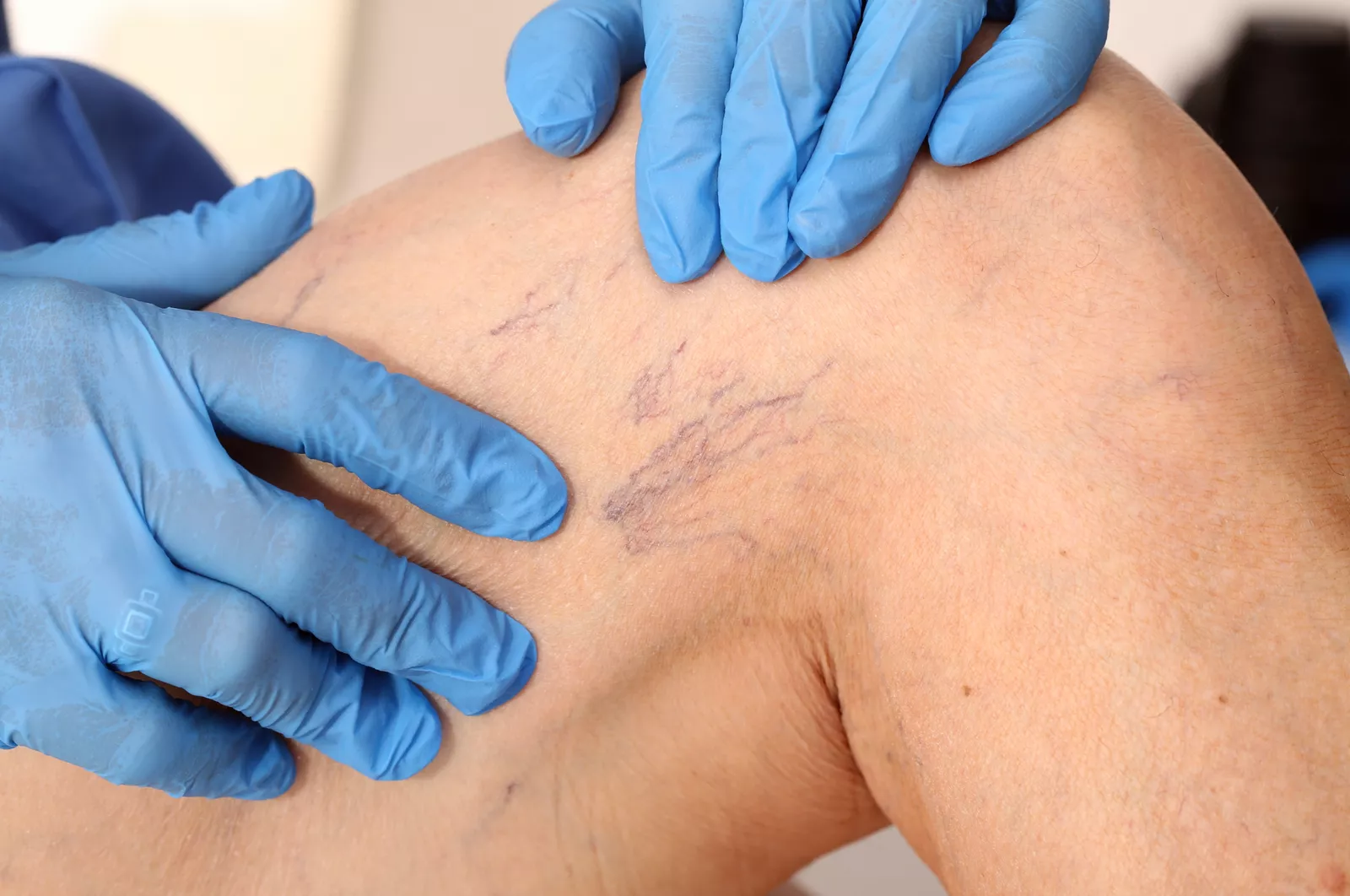
The primary cause of venous leg ulcers is chronic venous insufficiency (CVI), where inadequate blood circulation in the veins stems from faulty valves or a weakened calf muscle pump. This leads to blood pooling and increased pressure, damaging surrounding skin tissue. Approximately four in five venous leg ulcers are linked to varicose veins and circulatory insufficiency, according to Dr Mark Bratby, a consultant interventional radiologist at VeinCentre. Key risk factors include an ageing population, obesity, previous deep vein thrombosis (DVT), varicose veins, difficulty walking or immobility, previous leg injury or surgery, family history, pregnancy, and phlebitis.
Early symptoms can include aching, swelling, itching, skin discolouration and hardening of the skin around the affected area. Wounds may be slow to heal, produce a foul-smelling discharge and become infected. If left untreated, venous leg ulcers can lead to serious complications, including infection, sepsis and, in severe cases, limb loss — although it is very rare for venous ulceration alone to necessitate amputation. Dr Bratby issued an urgent appeal for greater public awareness. “Venous leg ulcers are a serious but often overlooked condition that can have a profound impact on a patient’s quality of life,” he said. “What’s concerning is that many of these cases are preventable with earlier diagnosis and treatment.” He warned that many people live with symptoms like aching, swelling or varicose veins for years without recognising them as early warning signs. “If these symptoms are ignored, the skin can begin to break down, eventually leading to a chronic wound that is much harder to treat.”
Conventional treatments such as compression therapy target symptom management but, as Dr Bratby cautions, they fail to tackle the fundamental problem of venous insufficiency. “Treating the underlying venous insufficiency is key to improving outcomes and reducing the risk of ulcers returning,” he said. Interventions such as endovenous laser ablation (EVLA) and foam sclerotherapy are used to seal damaged veins.
New Research: High-Intensity Exercise for Vascular Health
A major new study from Spanish researchers has found that high-intensity interval exercise (HIIE) may outperform other forms of physical activity in improving the function of blood vessels — a finding with potential relevance for conditions rooted in circulatory failure, including venous leg ulcers. Researchers from Miguel Hernández University of Elche and ISABIAL analysed 37 separate studies involving nearly 7,000 patients with coronary artery disease or chronic heart failure to determine what happens inside blood vessels during intense bursts of exercise.
Endothelial function — how well the blood vessels expand and contract — is a critical measure of vascular health. When the body is pushed hard and then recovers quickly, the rapid fluctuations in blood flow create what scientists call shear stress: essentially, friction against the vessel walls. The body responds to this stimulus by producing more nitric oxide, a molecule that keeps arteries relaxed and healthy. This process, known as flow-mediated dilation (FMD), is a key indicator of endothelial function.
The research indicates that HIIE consistently produces greater improvements in FMD than moderate-intensity continuous exercise, and does so in less total exercise time and with lower energy expenditure. “HIIE appears as the most robust option based on current evidence,” said Professor José Manuel Sarabia of Miguel Hernández University, who co-led the research. “It consistently outperforms moderate-intensity continuous exercise in improving vascular function.”
The findings extend beyond patients with heart conditions. Studies elsewhere have shown that high-intensity interval training can improve endothelial function in people with obesity, type 2 diabetes and type 1 diabetes. While the Spanish research was not directly focused on venous leg ulcers, experts note that any intervention that enhances nitric oxide production and supports blood vessel health could, in principle, address the circulatory insufficiency driving venous leg ulcer formation.
Varicose veins, a major risk factor for venous leg ulcers, affect an estimated 30-40% of the UK population at some point in their lives, with prevalence potentially exceeding 60% in those over 75. Treatments for varicose veins have evolved towards minimally invasive procedures, yet the National Wound Care Strategy Programme has highlighted a lack of coordinated data across the UK, hindering research and service planning. Chronic wounds are on the rise, partly due to an ageing population and increased comorbidities, and a significant number of leg ulcers have no recorded diagnosis — suggesting many patients may not be receiving effective care.

