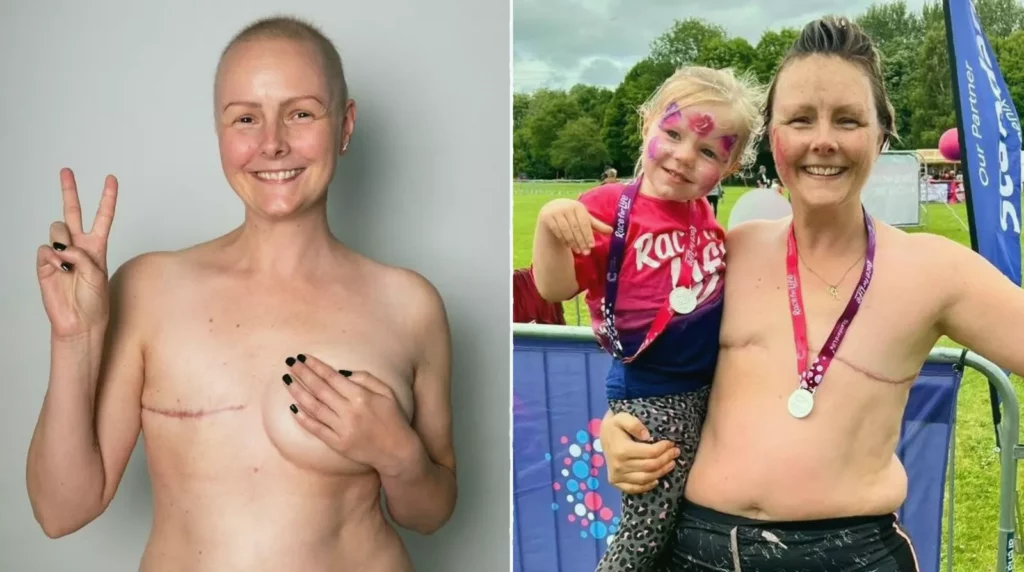
For Gemma Fish, the first warning that something was wrong wasn’t the discovery of a lump, but the unsettling, gradual shrinkage of her own breast—a change she mistakenly wrote off as a lingering effect of pregnancy.
The 43-year-old charity worker from Salford gave birth to her daughter, Rosie, at the end of 2021. Over the following year, her right breast continued to reduce in size, eventually becoming three cup sizes smaller than her left. It was only when her nipple inverted 14 months later that she sought medical help. On 17 February 2023, she was diagnosed with breast cancer.
“I put it all down to pregnancy changes,” Gemma said. “I purely just thought [a symptom] would be finding a lump… I didn’t know that changes in breast size was a potential symptom.”
A diagnosis that escalated
Initially diagnosed with stage one cancer, Gemma was told her right breast had shrunk to the size of the tumour lying beneath her skin. She underwent a single mastectomy, followed by aggressive chemotherapy and radiotherapy. In January 2024, she learned her cancer was “oestrogen fed,” leading to the removal of her ovaries. Tests on that tissue revealed the disease had spread, upgrading her diagnosis to stage four—metastatic cancer that is treatable but not curable.

“Living with stage four cancer is completely different now compared to how it was years ago,” Gemma said. “It’s no longer a straight death sentence… there’s lots of ladies that live long lives on various different treatment lines.” The five-year survival rate for stage four breast cancer in the UK is approximately 28%, according to national statistics.
Why a breast can shrink
Gemma’s case underscores a lesser-known sign of the disease. While lumps are the most recognised symptom, breast shrinkage can occur when a tumour develops within or behind breast tissue. Medical experts explain that some tumours, particularly those that are invasive, can pull on ligaments or structures within the breast, causing retraction and making the breast appear smaller or misshapen. This change, distinct from general asymmetry, is a physical distortion caused by the tumour’s presence.
This symptom is part of a broader spectrum of changes that warrant investigation. These include skin puckering or dimpling (often compared to orange peel), redness, a rash, nipple inversion or discharge, persistent breast pain, and swollen lymph nodes in the armpit. A rare but aggressive form called inflammatory breast cancer can also present with swelling and red, scaly skin.
Gemma’s cancer was identified as oestrogen receptor-positive (ER+), meaning it uses the hormone oestrogen to grow. Treatment often involves hormone-blocking therapy, though tumours can become resistant over time.
“If in doubt, get it checked out”
Following a second mastectomy and deciding against reconstruction, Gemma is now adjusting to life “flat chested,” a significant physical and mental adjustment. Her focus is on living as happily as possible with her young daughter. Her urgent message to others is to act on any change, no matter how minor it seems.
“If I had not ignored it and not buried my head in the sand it would have been caught a hell of a lot sooner,” she said. “The whole treatment plan would have been completely different… and possibly avoided it spreading.”

She echoes the guidance of the charity CoppaFeel!, which promotes regular self-checks. The charity advises people to systematically “look and feel” their chest area monthly, from the armpits to the collarbone, noting any changes in size, shape, skin texture, or nipples. Their core message is simple: know what is normal for you, and “if in doubt, get it checked out” by a GP.
The scale of the disease in the UK provides stark context for this advice. Cancer Research UK reports around 56,900 new breast cancer cases each year. A woman is diagnosed every nine minutes, and with projections suggesting this will rise to one every eight minutes by 2040, awareness of all symptoms is critical. Breast cancer remains a leading cause of death, with metastatic breast cancer being the primary cause of death in women aged 35-64 in the UK.
For Gemma, the lesson learned through her arduous journey is unequivocal. “It’s better to be safe than sorry,” she urges. Her story is a potent reminder that vigilance extends far beyond the search for a lump.