In a triumphant return to the stage she once dominated, Céline Dion has announced a series of comeback concerts in Paris, marking her first live performances since revealing her diagnosis with a rare and debilitating neurological disorder.
The star, who turned 58 this week, made the announcement on French television, telling viewers on France 2: “This year, I will receive the best gift of my life. I will have the chance to come and see you and to sing for you again in Paris starting this autumn, in September.” The news was simultaneously projected onto the Eiffel Tower in a celebratory light show, capping an advertising campaign that had fuelled speculation across the French capital.
Return to the Arena
The concerts are scheduled for September and October at the Paris La Défense Arena, a venue with a capacity of 40,000, where Dion will perform her hits in both French and English. Pre-sale tickets were made available from April 7, with general sales beginning on April 10. This return follows the cancellation of her world tour in December 2022, a decision forced by her ongoing health battle. Speaking of her readiness now, Dion has said she is “feeling good, I’m strong,” and “so ready to do this.”
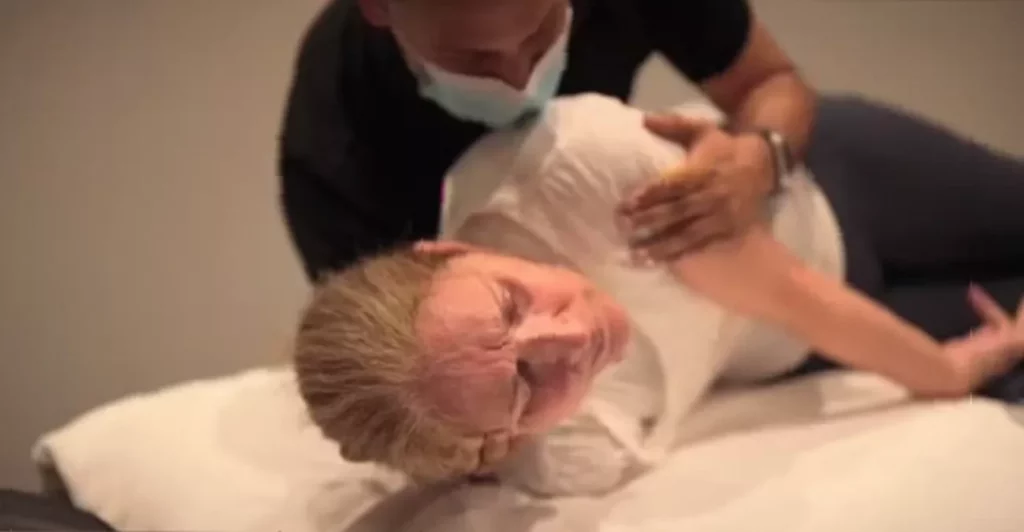
Her journey with the condition was documented with stark honesty in the Amazon Prime Video film “I Am: Celine Dion,” released in June 2024. Directed by Irene Taylor, the documentary, which became a top performer on the platform, showed the singer experiencing painful spasms and aimed to raise awareness of her diagnosis: Stiff Person Syndrome (SPS). Dion stated the film was a way to document her struggle and help others facing the same condition.
The Reality of Stiff Person Syndrome
SPS is a rare, progressive neurological autoimmune disorder, estimated to affect between one and two people in a million. The British Neurological Surveillance Unit identified 119 cases in the UK over a five-year period, supporting this prevalence figure. Despite its rarity, some experts believe it may be more common than thought, existing as a spectrum of disorders. It affects twice as many women as men, with symptoms typically emerging between the ages of 30 and 60.
The cause remains unknown, but research points to a faulty autoimmune response in the brain or spinal cord. The immune system mistakenly produces antibodies, often targeting an enzyme called glutamic acid decarboxylase (GAD). This disrupts the production of a crucial neurotransmitter, gamma-aminobutyric acid (GABA), which inhibits nerve activity. The result is hyperexcitable nerve cells, leading to the condition’s hallmark symptoms: severe, progressive muscle stiffness and violent, involuntary spasms.

These spasms often begin in the trunk and legs and can be triggered by seemingly minor stimuli—a sudden noise, an unexpected touch, cold temperatures, or emotional stress. This heightened sensitivity can lead to significant anxiety and phobias, including agoraphobia, as patients fear triggers in public spaces. Over time, the condition can force the body into hunched or abnormal postures, severely impair mobility, and cause an unsteady gait that increases the risk of frequent, dangerous falls. In severe cases, spasms can be powerful enough to fracture bones or dislocate joints, and involvement of chest muscles can lead to breathing difficulties.
Beyond the physical toll, non-motor symptoms like chronic pain, anxiety, depression, gastrointestinal issues, and cognitive impairment are common, significantly eroding quality of life and leading to social isolation. The condition is frequently associated with other autoimmune diseases, including type 1 diabetes, thyroiditis, vitiligo, and pernicious anaemia.
Diagnosis and Treatment: A Complex Path
Diagnosing SPS is notoriously difficult, often leading to years of misdiagnosis as Parkinson’s disease, multiple sclerosis, fibromyalgia, or even anxiety disorders. A definitive diagnosis typically requires a combination of clinical examination, blood tests to detect elevated levels of anti-GAD65 antibodies (present in up to 80% of classic cases), and tests like electromyography (EMG) to measure muscle activity. Imaging studies and lumbar punctures may also be used to rule out other conditions.
There is no cure for Stiff Person Syndrome. Treatment focuses on managing symptoms and may involve a combination of muscle relaxants, sedatives, anticonvulsants, and steroids to control spasms and stiffness. Immunotherapies such as intravenous immunoglobulin (IVIG) and plasmapheresis are used to modulate the faulty immune response. Supportive therapies are crucial; regular physical and occupational therapy help maintain mobility, while mental health support through Cognitive Behavioural Therapy (CBT) and mindfulness can help manage the associated anxiety and depression—though care must be taken, as some antidepressants can worsen symptoms.
In the UK, support for those affected is provided by organisations like The Brain Charity, which offers practical and emotional help for over 600 neurological conditions, and the dedicated Stiff Person Syndrome Support Group and Charity. The ongoing quest for better understanding and treatments is driven by research foundations investigating the precise role of autoantibodies in the disease.